EDOMETRIOSIS RESOURCE GUIDE: GENE EXPRESSION
To address endometriosis more effectively, we first need to understand what causes it. And it turns out it's not so simple.
The Biology of EndometriosisEndometriosis is a complex disease, which means that there is no single cause and no single answer. It is well known that endometriosis is very much linked to hormones, especially estrogen and progesterone. Gene expression research is providing many clues about other biological systems that contribute to endometriosis. These include inflammation and oxidative stress, processing of toxins – including chemicals called endocrine disruptors, blood vessels, and even repair of our DNA. While this can seem overwhelming , it’s also opening up new opportunities for better diagnostics, earlier detection, and more effective treatments by addressing the root causes.Gene Expression
Genes are sections of your DNA that carry the code for proteins that run everything that goes on in your body. On top of this, epigenetics is another layer that turns these genes on and off – like a light switch. Together, they support the proper functioning of our biology by ensuring that we are making the right proteins at the right time.
While endometriosis has a clear inherited genetic component, it is equally influenced by the environment. This means that the choices you make, along with the experiences and exposures you have in your lifetime, can impact how your genes and body function. Though you can’t change your genes, you CAN influence how they get expressed and thus affect your health – and potentially the health of future generations.
In this Endometriosis Resource Guide, you’ll learn simple strategies to optimize your body’s own biology. It’s a powerful tool to help you regain some control back from a disease that all too often feels like it’s controlling you.Simple Strategies to Transform Your Stress
Stress is everywhere, but what is it really? In a nutshell, stress is any influence on your physical, mental, emotional, or energetic systems that creates an imbalance. A small amount of stress is actually healthy.
Think about when you experience sore muscles in the early stages of a new exercise routine. The stress on your physical body gives a signal for the tissues to become stronger or more flexible.
Your body adapts and gets back into balance, better and healthier than it was before.
But feeling stressed over a long period of time is different. It depletes your body so that you don’t function at your best. You can’t think as well, your decision-making is off, your relationships suffer, and you feel too tired to do what you love.Whether it’s a nutrient deficiency, exposure to toxins, overexercising, difficulties in relationships, insufficient sunlight, sleep deprivation, hormonal imbalances … ANY imbalance in the system creates stress. Stress then creates downstream imbalances in every system linked to health – including inflammation and oxidative stress.
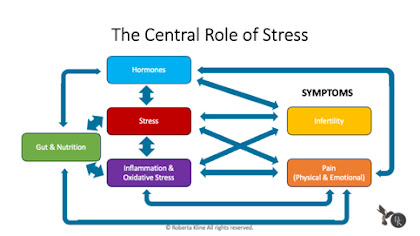
Stress and Endometriosis
In this graphic, you can see how stress is linked to every aspect of endometriosis. It is a central component that influences both your biology and symptoms. Because of this, it is a key part of any strategy to address your disease.
Your Personal Stress Blueprint
What bothers me isn’t what bothers you. Why is that? We are each unique in how we respond to stress. Uncovering your personal keys can transform how you approach stress - and your life.
Here are some simple strategies you can implement today. Each strategy can influence stress through gene expression and energetic balance. Together, they are much more powerful.
Your Guide to Healthy Gene Expression
Here are some simple strategies you can do to support and balance all of these biological systems, including stress, through healthy gene expression.
Eat Healthy Food
Food talks to our genes and provides critical support for biochemistry. The Mediterranean diet is the healthiest overall way to get what your body needs. Include more of the good stuff:
• Vitamins and minerals
• Phytonutrients
• Fiber
• Healthy fats and proteins
Minimize or eliminate the bad stuff:
• Processed foods
• Refined sugar
• Alcohol
Move Your Body
QMovement is more than exercise for weight or appearance. It’s part of a body-wide communication system, so aim for at least 60 minutes daily. Vary it and make it fun! Ideas include:
• Run, walk, hike
• Workout at gym
• Bike
• Swim
• Dance
• Gardening
• Play
Get a Good Night’s Sleep
Sleep is an active state of repair and regeneration, and is linked to every biological system through circadian rhythm. This means it’s not just about how much you sleep, but also when you sleep.
• Aim for 6-8 hours a night between 9 pm and 7 am.
• Avoid night shifts and frequent travel across multiple time zones.
• Address issues that interfere with sleep including snoring, sleep apnea, and restless legs.
Minimize Toxins
Toxins directly and indirectly damage DNA and alter biological processes. Minimize your exposure to endocrine disruptors and other toxins found in many places including:
• Pesticides
• Home cleaning products
• Plastics
• Personal care products
• Air and water pollution
• Smoking
• Medications
Manage your Stress
Stress is a response to internal and external events, including thoughts, beliefs, and trauma.While you cannot avoid stress, there are many strategies for managing it so it doesn’t have a big impact. Here are some common ones; find what works for you. It’s good to practice several approaches so you always have the right tool at the right time:
• Meditation
• Massage
• Energy work
• Creative outlets
• Nature, Pets
• Connection & Hugs
• JOY
Love yourself. Create your best life!
ULTRASOUND DIAGNOSTICS OF ENDOMETRIOMA
Endometriosis starts in the endometrium with abnormal cellular proliferation. Through the use of 3D Ultrasound, this disorder can be measured through the monitoring of the widening or the increased tissue in the endometrium. Another form of quantitative measure is by the study of blood flow in the endometrium. Its ability to spread can be recognized by the number of vessels in the active tissue. The big problem with staging endometriosis (or endometriomas) are the cysts that follow it. Because of its capacity to spread in most areas of the body, a strategic protocol for clinical management is to conduct IMAGE GUIDED treatments, whereby use of real-time scanning of or during therapeutic process helps navigate the focus the treatment area. Imaging solutions include CT (which has radiation), MRI, or the 3D Doppler ultrasound. CASE REVIEWS: We recently had a case where the endometriosis had metastasized under the arm. We've seen it metastasize in post-op scars. We can see the endometrial tissue block the ureters- hence, blocking the kidneys and destroying the kidney function. Moreover, the scars can cause bowel obstruction. While it's not categorized as malignant, it certainly can be deadly (as well as a seriously painful and debilitating disease). Women (especially those in advanced age groups) have expressed being completely incapacitated for three out of four days during their menstrual cycle. A vast majority of them also claimed experiencing mental health issues because of the pain and discomfort. The following slides are from Dr. Robert Bard's lecture presented in 2016 for the obstetrics and gynecology department at Mount Sinai Medical Center in New York City (ref: prior lecture from Harvard Medical School/the American Institute of Ultrasound in Medicine).
Use of the modern image guided treatment technologies offer non-invasive blood flow technology, which quantifies the aggression, either the aggressiveness of an inflammatory process like endometriosis or the invasive and metastatic potential of cancers such as endometrial cancer & cervical cancer. FIG-1: Upon observation, this it is not a primary bladder cancer. This is an inflammatory mass because the vessels are smooth (cancer vessels are wrinkly)- and there is a visible difference between the two. This is a three dimensional pelvic floor doppler study of the pelvis. If we start with scan A, we see the uterus on the bottom half and the bladder on the top, which is black, and within the black fluid is a mass. By looking below that, we see the (scan C and D) the abnormal blood vessels of the endometriosis. Hence, inflamed tissue is vascular and the same pattern of blood vessels from the abnormal endometrium is also in the bladder, indicating that the endometrial tissue has either invaded or metastasized into the base of the bladder. The two scans (B & D) show the bladder wall is intact. Hence, these are endometriosis that has metastasized or spread to the base of the bladder.
Notice the 3D images on the left with the red circle (Scan A) is the endometrial cyst, which is black, and the circle shows a small nodule within the cyst. What's important with this as contrasted to the previous study is this is NOT VASCULAR, which means this is inactive or subclinical at this time. On the right (E,F,G,H), we see that the pedicle that's going to the cyst and feeding the cyst, the area has multiple blood vessels in it. Because we're using 3D volumetric technology, we are able to quantify the number of vessels in the pedicle. The more blood vessels in the pedicle, the more aggressive the disease is. So back to the cyst. The cyst, there were no vesicles, but the pedicle feeding the cyst had a 13% ratio of blood vessels to assisted tissue. EPILOGUE Traditional medicine has not assisted with the mental depression, the anguish of the certainty that the pain will be monthly and the possible side effects including infertility. Since we've been using targeted therapies with lasers and focused ultrasound energies years ago, we are now globally using bioenergy treatments that is the near infrared laser and the pulse electromagnetic fields to calm down the process of this inflammatory disorder. |
Introduction: by Roberta Kline, MD
 Under a joint report with the Women's Diagnostic Network and HealthTech Reporter, our editors met with Ms. MJ Smith, a clinical ambassador from Screen Point Medical (breast imaging AI) at the 2023 NYC Roentgen Society conference. At the height of the medical conference, we found MJ to be a uniquely profound and engaging speaker about women's health topics. Exploring a private connection opened us into a collaborative and educational journey befitting our UNDERDIAGNOSED WOMEN series where MJ is truly a life-long supporter of diagnostic care, innovation and non-invasive options.
Under a joint report with the Women's Diagnostic Network and HealthTech Reporter, our editors met with Ms. MJ Smith, a clinical ambassador from Screen Point Medical (breast imaging AI) at the 2023 NYC Roentgen Society conference. At the height of the medical conference, we found MJ to be a uniquely profound and engaging speaker about women's health topics. Exploring a private connection opened us into a collaborative and educational journey befitting our UNDERDIAGNOSED WOMEN series where MJ is truly a life-long supporter of diagnostic care, innovation and non-invasive options.
Endometriosis (sometimes called "endo" for short) is a common health problem in women that is reported to affect more than 11% of American women between 15 and 44. It gets its name from the word endometrium, the tissue that normally lines the uterus or womb. When this tissue is found in locations outside of the uterus, it is called endometriosis. Most often this involves the nearby organs and tissues – ovaries, fallopian tubes, outer surface of the uterus, bladder, bowel and rectum. It can also be found in other locations including the vagina, cervix, vulva, or even distant tissues such as the lungs, brain, eye, and skin. Just like the lining of the uterus, this tissue responds to cycling hormones to grow. But unlike normal endometrium, it is not limited to the surface and does not shed. Because of this, it builds up and creates inflammation, scarring, and other changes that contribute to the most common symptom: pain.
While endometriosis is most often diagnosed in women in their 30s and 40s, it likely develops much earlier. Due to the wide range of symptoms that women can experience, and lack of effective and noninvasive diagnostic tools, women often suffer for years or even decades. Currently the only accepted way to diagnosis endometriosis is to directly visualize and biopsy the lesions with surgery. This is limiting for two reasons. First, endometriosis has to be considered as a possible explanation for symptoms that are often seen as “normal” for menstruating women. Second, the risk of not knowing has to outweigh the risk of potential complications of invasive surgery.
Endometriosis can also make it harder to get pregnant, and it is not uncommon for a diagnosis to be made only as part of evaluation or treatment for infertility. Getting a diagnosis to explain symptoms is only the first step in addressing endometriosis, however. There is no cure, and most current treatments often come with significant risks or side effects but do not fully resolve a woman’s symptoms. While research progresses slowly, we still do not have a clear understanding of what causes endometriosis, how to diagnose it early without invasive procedures, how to ease symptoms, and ultimately treat and possibly cure the disease itself.
This special interview features great insight from a woman’s journey with endometriosis. We explore her remarkable quest for answers from the range of pain relief to therapeutic treatments to risks of surgical solutions.
LIVING WITH ENDOMETRIOSIS:
From an interview with MJ Smith
 My personal and professional missions are both in women's health. By day, I work for a breast AI company focused on helping radiologists find breast cancers on mammograms. I chose this path because I believe in advancing causes that support women's health simply because women are core members of our culture and our families. I have had two family members, both maternal aunts, who died of breast cancer, - one at the age of 36, and an the other at the age of 52.
My personal and professional missions are both in women's health. By day, I work for a breast AI company focused on helping radiologists find breast cancers on mammograms. I chose this path because I believe in advancing causes that support women's health simply because women are core members of our culture and our families. I have had two family members, both maternal aunts, who died of breast cancer, - one at the age of 36, and an the other at the age of 52.
Advocacy for Endometriosis is directly related to my personal journey. Growing up with endometriosis since puberty, I've been to the emergency department probably over 20 times for pain or pelvic pain related conditions. The pain had me flat on my back for days at a time or falling out of bed with pain. I drove myself to a Planned Parenthood in Minnesota where I grew up and was prescribed birth control to manage it well into my twenties. Despite the hormonal treatments, I still had a series of episodes.
Endometriosis is the uterine tissue that grows and implants itself outside of the uterus. Going through that pain is the result of a complex process, resulting in swelling and bleeding inside the interstitial spaces of my body. Women who have endometriosis also often develop painful cysts on their ovaries.
I think the biggest reason you see women in the ER is pelvic pain. Women with chronic pelvic pain (which is often what endometriosis causes) are underserved by the healthcare community because we're constantly complaining of pelvic pain. The ER is not where you want treatment because you see a different doctor every time you get admitted. With emergency imaging, you usually get a pelvic ultrasound where cysts can show up and they're quick to assume that you have a cyst, or a cyst has burst and this is why you're uncomfortable. I think now you can do a pelvic MRI with contrast media- but it's still not enough to offer a definitive diagnosis. (To be continued below)
I found in the 20 years of suffering endometriosis that the only way to get a true diagnosis has remained to be a laparoscopic or an open pelvic surgery. It's incredibly difficult.
I know another woman who struggled through over seven years of infertility and it was only after seven years, and by then she was well into her late thirties or early forties, that she had surgery to identify endometriosis. Only then was that woman able to get pregnant. I have had a similar experience. I wasn't suffering infertility, but I was in so much pain in my late twenties that my doctor recommended a laparoscopic exploratory surgery because the pain is was so severe. I remember I was prescribed a month's worth of Vicodin leading up to the surgery. I am not a person who developed an addiction to pain medicine- but in retrospect this was done in the time when the entire country fell into a pandemic of addiction to pain medicine. I wouldn't have gotten that prescription in this day and age in 2023 if I have pelvic pain. Overall, there's no relief for me and over-the-counter meds that do not help. I just thank God I didn't develop an addiction after having taken Vicodin multiple times a day for a month leading up to that surgery... where, in fact, I was diagnosed with stage four endometriosis.
One of my ovaries was almost lost due to endometriosis. My doctor was able to keep that ovary and as a result I was able to get pregnant with my first child. I had a second child years later but surgery comes with complications. To this day, at 44, I recently went to the emergency department because of pelvic pain and it's still something I live with. I do take hormones but I've given up on looking for answers from academic research because I think that, in my opinion, I don't think we've gotten very far. The choice of hormones have side effects like an increased risk of breast cancer or uterine cancer. I'm very interested in minimally invasive treatment procedures but I just think we've come to a standstill with the traditional medical community when it comes to endometriosis.
Sexist stereotypes that see women as 'emotional' and consequently medical staff doubt a physical basis for women's pain. Men are viewed as more 'rational' and when men say they are feeling acute pain, their symptoms are taken more seriously and considered to have a physical cause. This means women receive very different care for pain management and pain diagnosis. Researcher, Karen Calderone found that women are more likely given sedatives as an answer to complaints of pain and are perceived as being anxious.
Medical professionals focus on returning the woman to a state of being calm and not investigating the cause behind their pain. The sedatives can then make the women seem calmer from outside appearance, while their medical condition can continue to worsen as they remain undiagnosed. Undiagnosed endometriosis has enormous repercussions for a woman. Life altering heavy bleeding, cramping and pain can lead to infertility, anemia, and internal adhesions requiring surgery.
WOMEN’S HEALTH DIGEST
From the publishers of THE WELLNESS JOURNAL and the WOMEN'S DIAGNOSTIC NETWORK NEWS comes a consortium of IPHA'S top professional contributors in women's health & wellness advocacy. Subscribe to our latest community E-news forum and get the insiders news on pain therapeutics, diagnostics and lifestyle upgrades. We welcome special guest contributors from all modalities of healing - from practitioners, product innovators and researchers. Also, gain valuable insight from success stories of real people and their experience with WHAT WORKED for them! Get front row access to our latest headlines. Visit: WomensHealthDigest.org

























No comments:
Post a Comment